Your cart is currently empty!
Type 2 diabetes and metabolic disease are becoming epidemics in America. Over 1.4 million Americans are diagnosed with diabetes every YEAR! Over half of adults in America have diabetes or prediabetes. That is over 129 million Americans.
The root cause of insulin resistance is the overstuffed and inflamed adipose tissue (fat cells). To reverse insulin resistance, we must get into a negative fat flux (burn more fat than is being stored) as quickly as we can. Burning more fat and shrinking the fat cells restores insulin signaling and can enable you to have A1c levels and fasting glucose that are no longer in the diabetic range.
We have had tens of thousands of clients reverse their type 2 diabetes with diet and lifestyle changes. And you can do it too. This article outlines everything you need to know to get your A1c back into normal range and insulin back to normal levels.
Types of Diabetes
There are a couple types of diabetes. The first and most common (and the focus on this article) is type 2 diabetes. This is called insulin resistance where the body makes insulin, but the cells (primarily fat cells) are resistant to the insulin. This article will focus on this form of diabetes.
Type 1 diabetes is an autoimmune disorder where the pancreas doesn’t produce any insulin. While this form can also greatly benefit from a keto or low carb lifestyle by greatly reducing insulin needs, they will always need to take exogenous (external) insulin.
For about 10 years now Maria and I have been calling Alzheimer’s type 3 diabetes. It is insulin resistance of the brain. The cells of the brain have become glycated and resistant to insulin. Glycation is the process where a sugar molecule gets bound to a protein or lipid (fat) molecule. This is caused by high carb, and especially high sugar diets for long periods of time.
You need insulin to get fuels (fats and glucose) into the cells. The cells that are glycated don’t allow the cell to get fuel and the cell dies. This is why a ketogenic diet can be so helpful for Alzheimer’s. Ketones that are made when eating this way can be used in the cells for fuel in place of fat or glucose without the use of insulin, thus fueling the cells and preventing them from dying. This is also the one case where increasing ketones with exogenous ketones or MCT oils can be helpful to provide the brain with even more fuels.
One other form to note is PCOS which is essentially insulin resistance of the reproductive system. More on the in the article HERE.
Understanding the Biology of Insulin Resistance
Understanding the mechanisms that cause type 2 diabetes and insulin resistance is important. There are several possible mechanisms that lead to insulin resistance. By far the most common is exceeding your personal fat threshold (more on this later). There are different mechanisms that can contribute to the severity of insulin resistance. For example, glycation is likely a big contributor to type 3 diabetes (Alzheimer’s). But for the most common form of insulin resistance, what is commonly called metabolic syndrome, the cause is exceeding your personal fat threshold. Metabolic syndrome symptoms are high fasting blood glucose, high triglycerides, high blood pressure, high fasting insulin and sometime excess body fat.
This video is a great place to start for understanding the mechanisms.
Insulin resistance is primarily caused by over stuffed adipose (fat cells) tissues. This can also be called Exceeding Your Personal Fat Threshold. Let’s take a look at what personal fat threshold is.
Personal Fat Threshold
I remember being told that when we are young we make new fat cells but when we become adults, most people can’t make new fat cells anymore. You just fill them up more or shrink the ones you have. This is a really important mechanism for insulin resistance. Since the number of fat cells are limited, as you gain body fat the body can run out of places to put the fat.
This explains why someone who is thin can have type 2 diabetes. They don’t have many fat cells but the ones they have are all stuffed and inflamed. It also explains whey someone can be 100 pounds overweight but have little signs of type 2 diabetes (normal blood sugars, etc.) because they have a lot of fat cells and they aren’t all overstuffed yet.
Once you exceed your body’s personal fat threshold, bad things start to happen. Your body starts storing fat in your liver, pancreas and other places where you do not want fat stored. It is struggling to put the fat anywhere it can because the fat cells are insulin resistant and not accepting fat anymore. This is metabolic syndrome.
Focusing Too Much On Insulin Only Model
I want to point something out here that is commonly discussed with respect to insulin resistance. Many will focus on insulin as the problem and that high insulin is what caused you to gain weight. But that is more of the result. You gained weight so insulin had to rise to hold back all the stored fat (more on this later).
Focusing only on insulin with respect to insulin resistance or weight loss in general has a few issues. There are many keto experts who focus only on insulin and if insulin doesn’t rise, you won’t gain weight and will lose body fat. But there is a fundamental problem with this concept. You can and will gain weight if you eat enough low insulin foods, even just pure fat.
If this view of insulin were true, it would be impossible to gain weight eating low to zero carb, and that just isn’t true. I (Craig) eating primarily carnivore for managing my Lyme disease pain. I can easily gain or lose 20 pounds based on how much fat I eat. All while eating carnivore/zero carb and with fasting insulin below 5 (my fasting insulin is usually 4 or lower) and very stable blood glucose. Dietary Fat is a dial you adjust up for maintenance or gaining, down for body fat loss.
Dietary fat only has 2 places it can go. Passed right through you in the stool or absorbed into your body. This is biology 101.
Some keto “gurus” will say that it goes right through you. This just doesn’t make any sense form a biology or evolutionary perspective. Calories were precious back in our hunter gatherer days. If our body just dumped fat when you were eating a lot of it in the summer from all the animal you hunted, you would never make it through the lean winter months without stored fat. And if you flushed fat through your colon in larger amounts (over 10g a day) you will live on the toilet. Remember Olestra, the fat that went through people undigested (the infamous WOW chips) and they had to put a label on them warning of anal leakage, from an extra 10-20 grams of fat going through the stool. Studies also don’t support this idea. In THIS study there was no change in fecal output of fat when the dietary fat was 62 grams a day or 152 grams a day. It was constant and always about 8 grams a day.
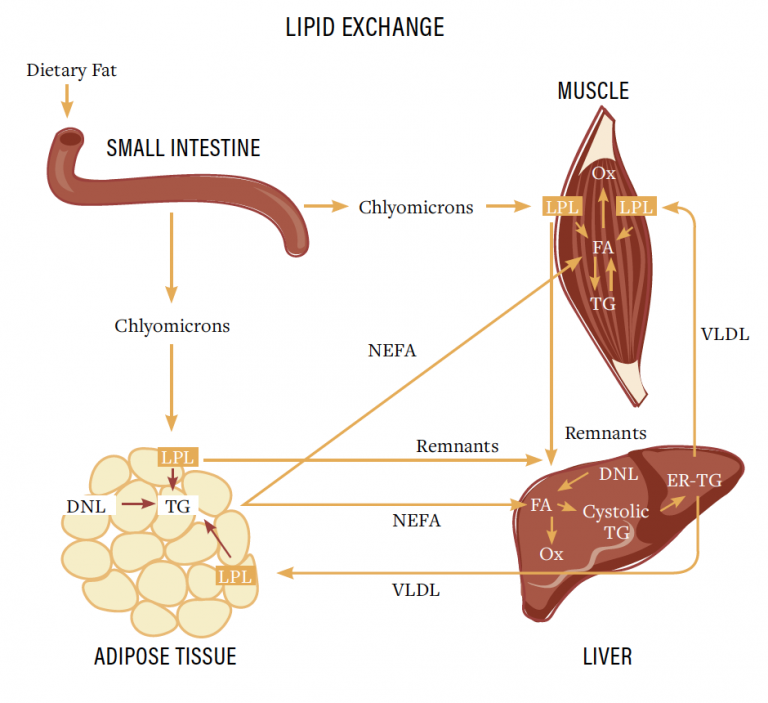
Almost all the fat in your diet ends up in your bloodstream. In this case it is either used as fuel, or stored in our fat cells. Unless you are in the middle of running a marathon, the vast majority of it will be stored in your fat cells. That is just how the body works.
But this biology shows there is another very dangerous effect of too little protein when it is combined with too much fat in the diet like with a fat fast.
Almost all fat that comes in through the diet end up in the bloodstream as chylomicrons. At this stage they have two fates, either be used as fuel in the muscle and other tissues or be stored in our adipocytes (fat cells). Studies have shown that most of the fat first goes to our fat storage before later coming out of fat storage and used as fuel. The mobilization of fat from your fat stores to be used as fuel is called lipolysis. Eating dietary fat will shut down lipolysis quickly as the body doesn’t want an over supply of fat in the blood.
So what puts fat into storage? There are a couple mechanisms. The main and primary controller is insulin. Yes, fat does raise insulin levels, not as much as protein or carbs, but it does raise insulin a bit. And in most people, that is enough to store it in your adipose tissue (fat cells).
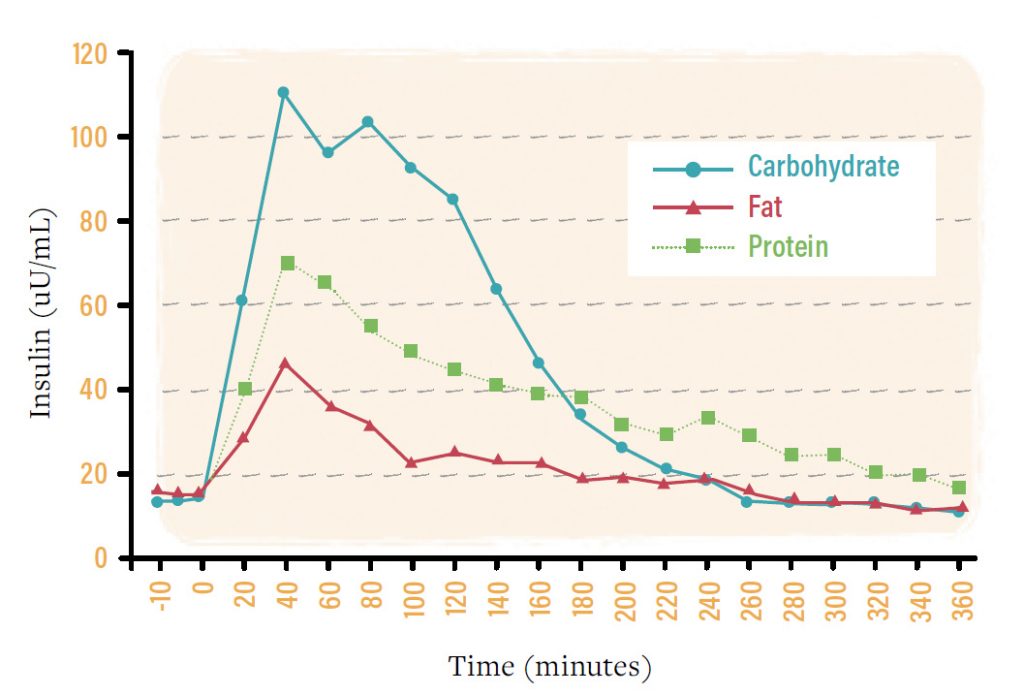
Insulin does two things. It helps store fuels (fat and glucose) into the tissues. Either muscle (glycogen) or adipocytes (fat). It also acts as a net to hold back fat or glucose from being released from the fat cells or muscle. This makes sense because if you have a large amount of glucose or fat coming in through the meal, the body doesn’t want an oversupply of fuel in the blood so it stops adding fuel (stops lipolysis) and starts storing it to lower the blood fuel levels.
Fats are also devoid of essential nutrients. Instead of drinking a cup of fatty coffee of butter, cream and coconut oil, I personally would eat a steak that actually gives me the satisfaction of chewing as well as nutrients to fill my body! Just look at how little vitamins and minerals there are in fat compared to the proteins.
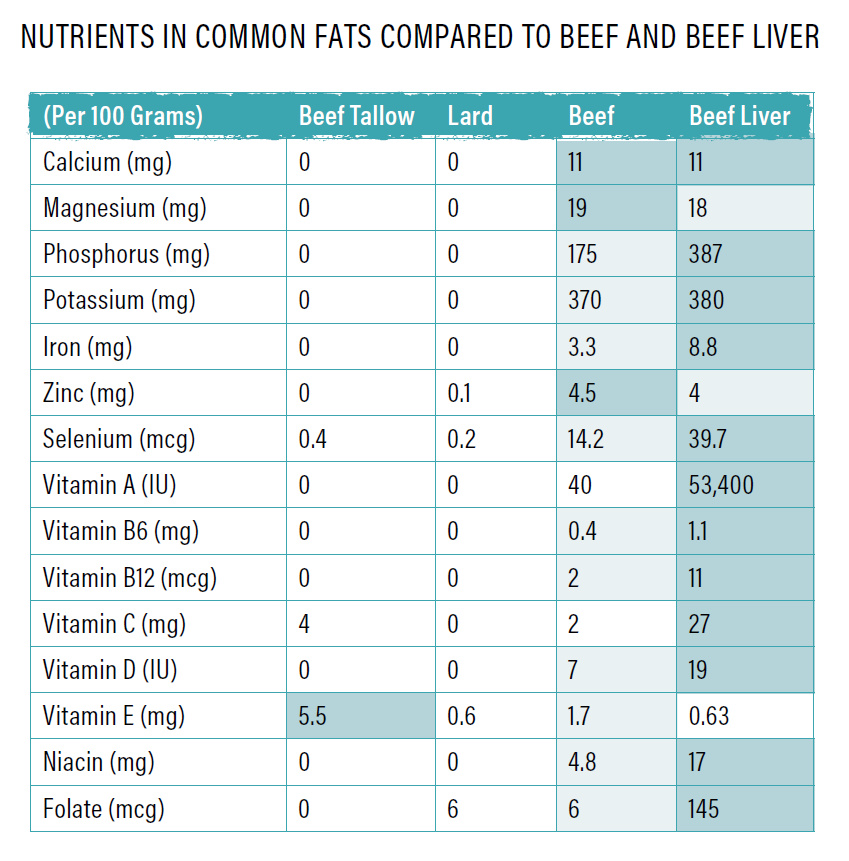
Other than a little vitamin A, fats have almost zero vitamins and minerals compared to the beef or other animal proteins. It’s not even close!
Animal proteins provide much more vitamins, minerals and complete proteins which are all important for reversing insulin resistance.
We are not saying to fear fats. We don’t fear fat and in maintenance consume lots of healthy fats from fatty ribeye’s and meats, some dairy in sauces, etc. But when fat loss and reversing insulin resistance is the goal and your body is already high fat, your diet doesn’t need to be high fat. Let your body use your own stored fat for fuel instead by dialing the dietary fat down. This will shrink the fat cells and reverse the insulin resistance at its root cause, the over stuffed fat cells.
Don’t Fear Protein
Protein isn’t to be feared, it is the cure.
There is a lot of talk about protein in the ketogenic community. Worries about “too much protein turning into glucose” are really a myth. Getting enough protein is very important for long term health. Maintaining lean mass as we age is very important. You don’t want to be wheelchair bound and frail when you are older. Achieving your protein goal or going over it is very important for quality of life as we age. As we age we need even more protein. This video describes what is happening with protein, especially with type 1 diabetics and gluconeogenesis.
Focusing on protein is also important for those with diabetes. You actually need MORE protein when insulin resistant. You need insulin to utilize protein and build muscle with it. If you have reduced insulin action (like with Type 1 diabetics) you need even more protein to ensure you get enough to maintain lean mass (muscle).
So don’t fear protein, embrace it. It is the key to reversing insulin resistance, keeping you strong as you age and giving glucose more storage space!
Getting Started
To reverse your insulin resistance you want to do two things. Shrink your fat cells and maintain or grow your muscle mass. This reverses the insulin resistance and lowers fasting insulin (shrinking fat cells and getting below your personal fat threshold) while giving glucose more place to be stored (muscle). In combination, these two things will help you reverse insulin resistance quickly.
Eat a well formulated ketogenic diet and spread protein out over your meals. Depending on how much insulin resistance you have, you might want to consider spreading out your protein over your meals. You still want to hit your protein goal; just don’t get too much protein in one meal to not put too much load on your insulin. And if you are type 1 or over 50 years old, you want even more protein every day.
1. Greatly Reduce Carbohydrates Intake
The best thing to rapidly bring down blood glucose is to greatly reduce your dietary carbohydrates. This will bring blood sugars under control quickly, but it won’t reverse the root causes by itself (over stuffed fat cells). It also brings the benefit of reducing hunger. This is the power of a low carb diet. When you cut the sugar and high carb foods, you get off the rollercoaster of hunger that make you feel the need to eat every couple hours. We recommend keeping carbs to 20g or less total carbs per day.
2. Get Enough Protein
It is important to maintain your muscle while losing body fat to gain the most insulin sensitive possible. More muscle means more place for the glucose to be stored. Also, protein has a very high thermic effect (more on that HERE) which makes protien a powerful tool for fat loss. Make sure to get at least your protein goal every day, or worst case average out to your protein goal over the course of the week.
3. Reduce Fat Intake
As we discussed above, you want to shrink your fat cells to reverse the insulin resistance. Lowering the dietary fat means the body is forced to burn more body fat for fuel. This reduces body fat and shrinks your fat cells.
4. Add Strength Training
Adding strength training can be another great tool for reversing insulin resistance. Having more muscle is great for increase insulin sensitivity and giving glucose more places to be stored.
Bonus: Add cold thermogenesis (cold therapy). This increases the amount of brown fat. The more brown fat you have, the more glucose it uses lowering blood glucose levels. Find out more about cold therapy HERE. Add intermittent fasting and try adding protein-sparing modified fasting (PSMF) days (1-3 days a week, more on PSMF HERE). This can help shrink fat cells faster and restore insulin signaling faster.
Getting your macros right is by far the most important step. All members have access to our macro calculator HERE. And platinum members can get personal macro targets HERE.
Supplements to Take
Diet and strength training are by far the most important things for reversing insulin resistance. But here are some supplements that can help.
Berberine: Berberine has been shown to help reduce blood sugar levels in some diabetics. Supplement with 1,000 milligrams twice a day.
Vitamin D: Optimize your vitamin D levels, which helps boost the immune system. Read more about vitamin D in the “High Blood Pressure” section (pages 123 to 125).
Magnesium glycinate: Magnesium is a miracle mineral, and about 70 percent of people are deficient in their magnesium levels (mainly because it takes 54 milligrams of magnesium to process 1 gram of sugar/starch!). Insulin stores magnesium, but if your insulin receptors are blunted and your cells grow resistant to insulin, you can’t store magnesium, so it passes out of your body through urination. Magnesium in your cells relaxes muscles. If your magnesium level is too low, your muscles will constrict rather than relax, which increases pain and decreases your energy level. Take 800 milligrams daily.
Zinc: Zinc is essential for creating DNA, supporting a healthy immune system, building proteins, and triggering enzymes. It also helps cells communicate by functioning as a neurotransmitter. As previously noted, taking zinc can make you nauseated, so we recommend starting slowly and ramping up your dosage by 10 milligrams a week until you can take 50 milligrams once a day without being nauseated. Take zinc with your first meal of the day.
